All published articles of this journal are available on ScienceDirect.
Antibiotic Susceptibility Pattern of Enterobacteriaceae Isolated from Raw Meat and Ghanaian Coin Currencies at Cape Coast Metropolis, Ghana: The Public Health Implication
Abstract
Introduction:
The emergence and upsurge of Multiple Antibiotic Resistant (MDR) Enterobacteriaceae in the environment is a cause of concern as this can result in an outbreak and spread to healthcare settings. MDR Enterobacteriaceae have been associated with high morbidity and mortality due to delay in selecting and delivering active therapy in time.
Aims & Objectives:
The study was conducted to investigate the level of contamination of raw meat and Ghanaian coins in circulation at Cape Coast Metropolis. In all, 10 raw meat were sampled each from chevron and beef from Kotokuraba market, and 400 Ghanaian coin currencies retrieved from food vendors, students, transport operators and banks were used in this study.
Materials & Methods:
The Enterobacteriaceae species isolated were tested for their susceptibility to Ampicillin, Tetracycline (TET), Gentamicin (GEN), Cotrimoxazole (COT), Cefuroxime (CRX), Cefixime (CXM), Cefotaxime (CTX), Penicillin (PEN), Cloxacillin (CXC), Erythromycin (ERY) and Amikacin (AMK) antibiotics using Mueller-Hinton agar antibiotic diffusion technique. Of the isolated Enterobacteriaceae, 30% and 62% from chevron and beef respectively and 14.17%, 13.75% and 10.63% from food vendors, students and transport operators respectively showed resistance to some of the antibiotics tested.
Results & Discussion:
8.6% of the Escherichia coli (E. coli) isolated from chevon were resistant to CRXr-CHLr-AMPr-COTr-GEMr and 15.5% of CRXi-CHLi-AMPr-TETr-COTr from beef. 40.0% of E. coli isolated from coin currencies were resistant to CRXr-CHLr-AMPr-TETr-CTXr, 50.0% of Enterobacter spp to CRXr-CHLr-AMPr-TETr-CTXr, 16.67% of Proteus spp to CRXi-CHLi-AMPr-TETr-AMKi, 40% Pseudomonas spp to CRXr-AMPr-TETr-AMKi and 100% of Enterobacter spp to CRXr-AMPr-TETi-CTXr.
Conclusion:
The multidrug-resistant Enterobacteriaceae isolates from circulating Ghanaian coins and raw meats in the Cape Coast metropolis is an indication of an impending danger which requires immediate attention to prevent a possible outbreak and spread from the society to the hospital setting.
1. INTRODUCTION
Enterobacteriaceae strains are the major foodborne and waterborne pathogens which cause approximately 2 million deaths each year in the developing countries [1, 2]. The increasing spread of carbapenem-resistant Enterobacteriaceae could worsen the poor health conditions in the community within these countries [3-5]. The continuous isolation of low antibiotic sensitive Enterobacteriaceae pathogens from surfaces of objects including currencies, beef and chicken and other substances are well reported [6-8]. The faecal contamination of antibiotic-resistant Enterobacteriaceae such as Salmonella spp., Escherichia coli, Proteus, and Klebsiella species is a Major concern for food hygiene in developing countries such as Ghana [9].
The isolated Enterobacteriaceae from the environment in Ghana with decreased susceptibility to carbapenems require constant surveillance and the need to put in place measures to prevent a possible outbreak of antibiotic-resistant Enterobacteriaceae in Ghana [9, 10]. As such an outbreak can enter the primary healthcare system and cause infections in the hospital [11, 12].
Klebsiella pneumoniae, E. coli, Enterobacter spp., Pseudomonas aeruginosa, and Acinetobacter spp. have been shown to constitute major multi-drug resistant bacterial infections both in the community and hospital [13]. This multidrug-resistant Enterobacteriaceae have been isolated from the respiratory tract, urinary tract, bloodstream septic, post-surgical wound infections and pneumonia in the hospitals in Ghana [14]. A nationwide antibiotic resistant surveillance has reported over 70% antibiotic-resistance of all bacterial pathogens isolated from in-patient departments in Ghanaian hospitals [15].
Antibiotic resistances are associated with increased morbidity and mortality compared to antibiotic susceptible bacteria [16]. High mortality rates of up to 75% have been reported for bloodstream infection of antibiotic-resistant bacteria which are related to the delay in the timely selection and delivery of active therapy [17, 18]. In spite of the high burden of multidrug-resistant Enterobacteriaceae recorded in hospitals in Ghana, no obvious measures have been instituted to mitigate this surging problem [16].
Again, environmental isolation of multi-drug resistant Enterobacteriaceae has been sparsely reported in Ghana [19]. However, comprehensive data covering surveillance on antibiotic-resistant bacteria and their transmission pathways, assessment of transmission risk, policy implementation and monitoring across hospital and environment acquired infections are lacking in Ghana [16, 19]. A similar observation was made by WHO in a recent review indicating lack of quality data on prevalence, level of resistant bacteria, isolation and characterization of bacterial resistance genes across humans, animals, food and community-acquired infections in low-income countries like Ghana [20]. The lack of evidence in the rapid emergence and dissemination of multi-resistant Enterobacteriaceae between the environment and hospital domains is a major challenge to awareness creation, effective management and implementation of appropriate control measures against drug-resistant bacterial infections in Ghana [21].
This study was conducted to assess the antibiotic susceptibility patterns among Enterobacteriaceae isolates from raw meat sources and Ghanaian coin currencies in Cape Coast Metropolis, the regional capital of the Central region of Ghana. We report multiple antibiotic resistance patterns of the isolated Enterobacteriaceae in this study as a baseline data for future studies on the transmission dynamics of multiple resistant Enterobacteriaceae in Cape Coast, Ghana.
2. MATERIALS & METHODS
2.1. Study Area
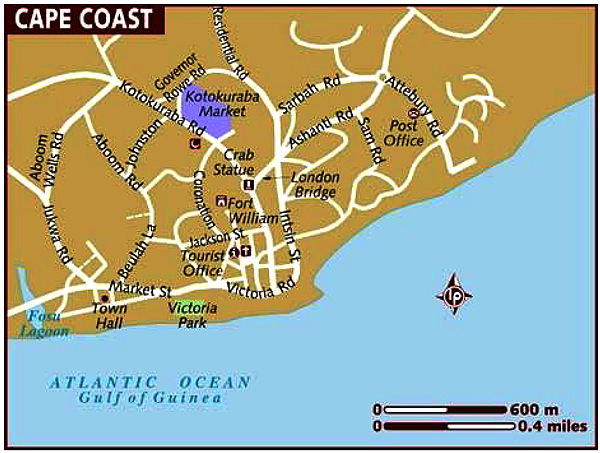
The study was conducted in Cape Coast Metropolis located in the central region of Ghana. Bacteria samples from freshly prepared meat from goat and cattle were taken from the slaughterhouse at Kotokuraba market, the main meat supplying source for the Cape Coast Metropolis and its neighbouring districts which covers an area of 122 square kilometres. Bacteria on coin currencies were also sampled from the University of Cape Coast campus and its environs which is located about five kilometres from the Kotokuraba market (Fig. 1).
2.2. Sample Collection from Meat and Coin Currencies
Freshly sacrificed meat of goat and cattle ready for the market was sterile swabs; 10 each from the slaughtering house at Kotokuraba market. Each sample was collected in duplicates from the flesh and the offals per meat. The samples were aseptically transported on ice to the microbiology laboratory and stored at 4°C in a refrigerator.
A total of four hundred (400) Ghanaian coin currencies; three hundred and sixty (360) coins currencies in circulation were randomly collected from food vendors in the market, transport operators, and students together with forty (40) non-circulating coins currencies from the bank located within the University Cape Coast campus were aseptically collected and transported to the microbiology laboratory of Biomedical Sciences, University of Cape Coast and stored at 4 °C in a refrigerator.
2.3. Microbiological Analysis
2.3.1. Bacteria Isolation
All the samples were sterilely swabbed and dipped into sterile buffered peptone water for 12-16 hours at 37oC in a shaking incubator. The inoculums were sterilely streaked uniformly on Blood agar (Sigma-Aldrich) and MacConkey agar (Sigma-Aldrich) plates using wire loops and incubated at 37oC overnight to allow for bacteria growth [22]. All Gram-negative, catalase positive, and oxidase negative isolates were further examined.
2.4. Biochemical Identification
Pure colonies were selected and sub-cultured on nutrient agar slant and were further processed for biochemical tests. Well-known traditional biochemical tests and selective media for bacteria identification were employed [23]. The isolates were identified using Endo agar (Sigma-Aldrich), MacConkey broth (Sigma-Aldrich), and Simmons citrate agar (Sigma-Aldrich), catalase, coagulase, oxidase, sugar fermentation (Triple sugar iron (TSI) agar), indole, citrate utilization, urease production, and motility tests. The identified bacterial species were kept in a 20% glycerol/medium mixture at −80 °C at the microbiology laboratory of Biomedical Sciences, University of Cape Coast, Ghana.
2.5. Antibiotic Susceptibility Test (AST)
Pure colonies were picked, emulsified in normal saline and compared with 0.5 McFarland solution to measure the bacteria turbidity [24]. Mueller-Hinton agar antibiotic diffusion technique (Kirby-Bauer NCCLS modified disc diffusion technique) was used for antibiotic susceptibility [25]. Ampicillin (Amp) (10μg), Tetracycline (TET) (10μg), Gentamicin (GEN) (10μg), Cotrimoxazole (COT) (25μg), Cefuroxime (CRX) (30μg), Cefixime (CXM) (30μg), Cefotaxime (CTX) (30μg), Penicillin (PEN) (10IU), Cloxacillin (CXC) (5μg), Erythromycin (ERY) (5μg) and Amikacin (AMK) (30μg) antibiotic discs were used to test for susceptibility of the isolated bacteria to the commonly used antibiotics. The dried Mueller Hinton agar plate was plated with the isolated microbes. The appropriate antimicrobial-impregnated disks were placed on the surface of the agar using sterilized forceps and incubated at 35oC overnight. The antibiotic inhibition zones were measured to the nearest millimetre (mm) from the centre of the disk to a point on the circumference of the zone where a distinct edge was seen using a rule. The obtained values were multiplied by 2 to obtain the diameter of the inhibition zone.
3. RESULTS
Enterobacteriaceae isolates from chevron (30%) and beef (62%) were resistant to some of the antibiotics tested. 120, 80, 160, and 40 of Ghanaian coin currencies were collected from food vendors, students, transport operators and the banks representing 30%, 20%, 40%, and 10%, respectively. E. coli, Enterobacter spp, Shigella spp, Klebsiella spp, Pseudomonas spp, Enterobacter spp, and Proteus spp were the Enterobacteriaceae isolates from the sampled coin currencies. Among the isolates, 4.17%, 3.75%, 1.25%, and 0% had multiple antibiotic resistance while 6.67%, 6.25%, 1.25% and 0% were sensitive to the antibiotic tested among the E. coli isolates from food vendors, students, transport operators and the bank, respectively. The isolation of Enterobacter spp, Shigella spp, Klebsiella spp, Pseudomonas spp, Enterobacter, spp and Proteus spp also showed multiple antibiotics resistance (Table 1).
| Antibiotic Non-Susceptible Pattern of Isolates | Food Vendors | Students | Transport | Bank | |
|---|---|---|---|---|---|
| N (%) | N (%) | N (%) | N (%) | ||
| Escherichia coli | Pos | 5 (4.17%) | 3 (3.75%) | 2 (1.25%) | 0 (0.0%) |
| Neg | 8 (6.67%) | 5 (6.25%) | 2 (1.25%) | 0 (0.0%) | |
| Enterobacter spp | Pos | 1 (0.83%) | 1 (1.25%) | 2 (1.25%) | 0 (0.0%) |
| Neg | 3 (2.5%) | 7 (8.75%) | 12 (7.5%) | 0 (0.0%) | |
| Shigella spp | Pos | 0 (0.0%) | 0 (0.0%) | 0 (0.0%) | 0 (0.0%) |
| Neg | 1 (0.83%) | 1 (1.25%) | 1 (0.63%) | 0 (0.0%) | |
| Klebsiella spp | Pos | 1 (0.83%) | 0 (0.0%) | 1 (0.63%) | 0 (0.0%) |
| Neg | 5 (4.17%) | 2 (2.5%) | 9 (5.63%) | 0 (0.0%) | |
| Pseudomonas spp | Pos | 2 (1.67%) | 2 (2.5%) | 1 (0.63%) | 0 (0.0%) |
| Neg | 13 (10.83%) | 6 (7.5%) | 23 (14.38%) | 0 (0.0%) | |
| Proteus spp | Pos | 8 (6.67%) | 5 (6.25%) | 11 (6.88%) | 0 (0.0%) |
| Neg | 5 (4.17%) | 7 (8.75%) | 12 (7.5%) | 0 (0.0%) | |
| Total coins collected | 120 (30.0%) | 80 (20.0%) | 160 (40.0%) | 40 (10.0%) | |
The percentages of multiple antibiotic resistant Enterobacteriaceae isolated from meat sources (beef and chevron) and Ghanaian coin currencies were interpreted using clinical and laboratory standards institute (CLSI) breakpoints as shown in Table 2 and 3. In all, 4.8% and 8.6% of the E. coli isolated from chevon were resistant to Cefuroxime, Chloramphenicol & Ampicillin (CRXr-CHLr-AMPr) and Cefuroxime, Chloramphenicol, Ampicillin, cotrimoxazole and Gentamicin (CRXr-CHLr-AMPr-COTr-GEMr), respectively whereas E.coli from beef source showed 15.5% and 6.4% resistance to Cefuroxime, Chloramphenicol, Ampicillin, Tetracycline, and cotrimoxazole (CRXi-CHLi-AMPr-TETr-COTr) and Cefuroxime, Chloramphenicol, Ampicillin, Tetracycline, and cotrimoxazole (CRXr -CHLi-AMPr-TETr-COTr), respectively. 3.9% of Enterobacter spp; 2.7% of Proteus spp. isolates from chevron, 6.2% and 12.4% isolates from a beef source and 3.5% Pseudomonas spp. showed multiple antibiotic resistance (Table 2).
40.0% of E. coli isolated from the coin currencies were resistant to Cefotaxime, Chloramphenicol, Ampicillin, Tetracycline, and Cefuroxime (CRXr-CHLr-AMPr-TETr-CTXr); 50.0% of Enterobacter spp. were resistant to CRXr-CHLr-AMPr-TETr-CTXr; 16.67% of Proteus spp. resistant to CRXi-CHLi-AMPr-TETr-AMKi; 40% Pseudomonas spp. resistant to CRXr-AMPr-TETr-AMKi and 100% of Enterobacter spp. resistant to CRXr-AMPr-TETi-CTXr (Table 3).
| Isolates | Sources | Drug Resistant pattern | % isolates |
|---|---|---|---|
| Escherichia coli | GT1 | CRXr-CHLr-AMPr | 4.8 |
| Enterobacter spp | GT2 | CRXi-AMPr-COTr | 3.9 |
| Escherichia coli | GT3 | CRXr-CHLr-AMPr-COTr-GEMr | 8.6 |
| Proteus spp. | GT4 | CRXi-CHLi-AMPr-TETr-AMKi | 2.7 |
| Proteus spp. | BF1 | CRXi-AMPr-TETi | 6.2 |
| Proteus spp. | BF2 | CRXr-CHLi-AMPr | 12.4 |
| Escherichia coli | BF3 | CRXi-CHLi-AMPr-TETr-COTr | 15.5 |
| Pseudomonas spp | BF4 | CRXi-AMPr-TETr-CTXi-GENr | 3.5 |
| Escherichia coli | BF5 | CRXr-CHLi-AMPr-TETr-COTr | 6.4 |
| Isolates | Drug-resistant pattern | Number | % |
|---|---|---|---|
| Escherichia coli | CRXr-CHLr-AMPr | 1 | 10.0% |
| CRXi-CHLi-AMPr-TETr-COTr | 2 | 20.0% | |
| CRXr-CHLr-AMPr-TETr-CTXr | 4 | 40.0% | |
| CRXr-AMPr-COTr-CTXr | 3 | 30.0% | |
| Enterobacter spp | CRXi-AMPr-COTr | 1 | 25.0% |
| CRXr-CHLr-AMPr-TETr-CTXr | 2 | 50.0% | |
| AMPr | 1 | 25.0% | |
| Proteus spp | CRXi-CHLi-AMPr-TETr-AMKi | 4 | 16.67% |
| CRXi-AMPr-TETi | 2 | 8.33% | |
| CRXr-CHLi-AMPr | 4 | 16.67% | |
| CRXr-AMPr-TETr-CTXr | 8 | 33.33% | |
| CHLi-AMPr-COTi | 6 | 25.0% | |
| Pseudomonas spp | CRXi-AMPr-TETr-CTXi-GENr | 1 | 20.0% |
| CRXr-AMPr-TETr-AMKi | 2 | 40.0% | |
| AMPr | 2 | 40.0% | |
| Klebsiella spp | CRXr-AMPr-TETi-CTXr | 2 | 100% |
4. DISCUSSION
Antibiotic-resistant Enterobacteriaceae contamination of meat sources and circulating currencies had been widely reported [10, 25]. This suggests that meat sources and circulating currencies allow pathogens to disseminate and cause infections in the environment with possible transmission into hospital settings [26]. Multi-antibiotic resistance to β-lactams such as Ampicillin, Penicillin, and the first and second generation cephalosporins by Enterobacteriaceae have been isolated and reported in Ghana [27, 28]. The incidence of multi-antibiotic resistant Enterobacteriaceae poses a serious threat to the healthcare system in Ghana as these organisms can spread from the environment to the hospital setting leading to nosocomial infections. This study assessed the extent to which raw meat and circulating currencies in the Cape Coast Metropolis are contaminated with multi-antibiotic-resistant Enterobacteriaceae.
The high prevalence of multi-resistant E. coli and non-E. coli Enterobacteriaceae from raw meat and coin currencies in circulation at Cape Coast metropolis is an indication of the complex nature of emerging antibiotic resistance by Enterobacteriaceae and its implication on the limited resourced health facilities in the study area [29]. In this study, we isolated E. coli, Enterobacter spp, Shigella spp, Klebsiella spp, Pseudomonas spp, and Proteus spp with resistance to second and third generation cephalosporins, an effective antibiotic against Enterobacteriaceae species. This suggests selection and emerging resistance to extended-spectrum β-lactamase (ESBL)-producing Enterobacteriaceae in Cape Coast [30, 31]. ESBL resistant Enterobacteriaceae in circulation should be a major concern since this limit the timely selection and treatment of infections.
Enterobacteriaceae cause infection in the bloodstream, surgical sites, Urinary Tract Infections (UTIs), respiratory tract infections and also cause frequent infections in diseases such as cancer and diabetes [32, 33]. A similar occurrence of MDR Enterobacteriaceae between the hospital and community-acquired infections has been reported [34]. The readily and easily spread of MDR Enterobacteriaceae from contaminated animal food sources and contact surfaces makes it a public health concern [35].
Isolation of ESBLs resistant Shigella and E. coli from raw meat and currencies is a warning ahead of the impending danger of emerging antibiotic resistance in enteric bacteria, a major cause of acute diarrhoea [36-38]. Acute diarrhoea is a health problem that causes the highest morbidity and mortality in children in developing countries [39]. Shigella colonizes the colonic mucosa and induces invasion resulting in a spectrum of dysentery (shigellosis) disease even in a healthy person with a lower dose of infection [40, 41]. Similarly, pathogenic E. coli causes severe intestinal and extra-intestinal diseases such as hemolytic uremic syndrome in humans [42]. The faecal-oral route transmission of both Shigella spp. and pathogenic E. coli should be a concern of public health especially with emerging ESBL resistance in a poor sanitation environment since infection of these drug-resistant pathogens can spread through contaminated foods or drinking water and also by person-to-person contact [43, 44].
ESBL resistant Klebsiella and Enterobacter, the causative agents of a variety of infections such as respiratory, Urinary Tract Infections (UTI), bacteremia, sepsis, pneumonia, cystitis, pyelonephritis and lung abscess [45] were isolated from raw meat and currencies in this study. Klebsiella and Enterobacter infections are frequently acquired through hospital settings with multiple antibiotic resistant strains and they occasionally spread from the hospital environment into the community to cause infection in a healthy individual [46, 47]. The isolation of multiple ESBL resistant strains of Klebsiella and Enterobacter from coin currencies and raw meat requires prompt action to arrest its possible spread and spill-over unto the healthcare setting.
The isolation of uropathogens such as Pseudomonas and Proteus which are associated with polymicrobial infections during long-term catheterization [48]. The involvement of these pathogens in polymicrobial infections has been associated with high mortality among patients [49]. The extensive resistance to the beta-lactamase antibiotics limits the choice of drugs and treatment options among infected patients with reduced immunity due to sickness. In some cases, severe and permanent renal damage such as of the bladder and kidney stones, increase the severity of cystitis, pyelonephritis, nephrosis, urolithiasis, and bacteremia can result from the infections of P. mirabilis [50].
The multidrug-resistant Enterobacteriaceae isolates from circulating Ghanaian coins and raw meats in the Cape Coast metropolis are an indication of impending danger which requires immediate attention to prevent a possible outbreak and spread from the society to the hospital setting. The emerging Enterobacteriaceae with multiple ESBL resistant strains in the community require public health response as it has a tendency to spread from the community to the surrounding clinics. Although there are no current outbreaks of multidrug-resistant Enterobacteriaceae in Cape Coast, these resistant pathogens could rapidly expand and spread across the entire Central region and Ghana as a whole. Such an expansion would be detrimental to public health due to limited treatment options and worsen the clinical outcomes in Cape Coast metropolis and the entire country as a whole.
Constant surveillance of ESBL resistant and carbapenemase-producing CRE Enterobacteriaceae is required to estimate the incidence of infection, the risk of infection, cost and possible treatment options available for these multidrug-resistant pathogens. In addition, it is important to identify the sources and the routes of contaminations coupled to the pattern of spread of this drug-resistant Enterobacteriaceae in Cape Coast metropolis for a proper understanding of the dynamics involved and measures to prevent outbreaks in the community. It is also important to understand the mechanisms underlying drugs resistant Enterobacteriaceae isolated from coin currencies and raw meat sources to have an idea of the pattern of the spread of these drug-resistant strains.
CONCLUSION
In conclusion, we report the isolation of multiple antibiotic resistant Enterobacteriaceae phenotypes from raw meat sources and Ghanaian coin currencies in circulation at Cape Coast metropolis. The high levels of ESBL and MDR isolated from currencies from food vendors, transport operators, and students should be a public health concern since Enterobacteriaceae have the ability to transfer their resistant genes (mcr gene) among strains to confer resistance to colistin and tigecycline, the only effective therapeutic drugs against ESBL-E. This finding requires immediate public health measures to avoid epidemic outbreaks within the metropolis. Personal hygiene and measures for proper handling of currencies are advised to reduce the spread of drug-resistant bacteria in the metropolis.
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
Not applicable.
HUMAN AND ANIMAL RIGHTS
No animals/humans were used for studies that are the basis of this research.
CONSENT FOR PUBLICATION
Not applicable.
AVAILABILITY OF DATA AND MATERIALS
The authors confirm that the data supporting the findings of this research are available within the article.
FUNDING
None.
CONFLICT OF INTEREST
The authors declare no conflict of interest, financial or otherwise.
AUTHORS CONTRIBUTION
All authors contributed equally
ACKNOWLEDGEMENTS
We thank the staff and laboratory technologists of the Department of Biomedical Sciences, School of Allied Health Sciences, College of Health and Allied Sciences, University of Cape Coast, Ghana for their assistance during the laboratory work. We also thank Dr. Yeboah Kwaku Opoku for his critical review and the correction of the manuscript.


