All published articles of this journal are available on ScienceDirect.
Diagnostic Performance of Xpert MTB/RIF Assay Versus Ziehl-Neelsen Method for the Diagnosis of Pulmonary Tuberculosis in Addis Ababa, Ethiopia
Abstract
Background:
Worldwide Tuberculosis (TB) is the ninth leading cause of death from a single infectious agent, positioning on top of Human Immuno Deficiency Virus (HIV) and it is still an eminently serious public health problem. In developing countries, Ziehl-Neelsen (ZN)-stained sputum smear microscopy is the most widely used diagnostic method in diagnosing Pulmonary Tuberculosis (PTB). This study was aimed to compare the diagnostic performances of ZN-method with Xpert MTB/RIF assay for the diagnosis of PTB in Addis Ababa, Ethiopia.
Methods:
Facility-based cross-sectional study design was conducted from September 2016 to June 2017 on a total of 244 sputum samples collected from presumptive TB patients. The L-J sputum culture was used as a gold standard to compare the diagnostic performances of Xpert MTB/RIF assay and ZN-methods. Kappa values were analyzed by using statistical package for Social Science (SPSS) version 20 software at 95% Confidence Interval (CI). The Sensitivity, Specificity, Positive Predictive Value (PPV) and Negative Predictive Value (NPV) of ZN-stained sputum smear microscopy and Xpert MTB/RIF assay were calculated against the gold standard.
Results:
The Sensitivity, Specificity, PPV and NPV of ZN-stained sputum smear microscopy were 68.38%, 95.28%, 93.02% and 76.58% respectively, while for Xpert MTB/ RIF assay were 88.89%, 81.89%, 81.89% and 88.89% respectively. The results of the two diagnostic approaches were concordant with the gold standard with a kappa value of ZN 0.650 and 0.743 for Xpert MTB/RIF assay.
Conclusion:
This study concludes that the sensitivity of Xpert MTB/RIF assay was better than ZN-stained direct sputum smear microscopy for the diagnosis of pulmonary tuberculosis.
1. BACKGROUND
Worldwide, TB remains one of the global health threats [1]. In developing countries, TB case detection is hampered by less utilization of diagnostic technologies, lack of easy and cost-effective point of care laboratory diagnostics, lack of infrastructures, and laboratory staff capacities to handle high-volume workloads [2, 3]. As a result, ZN-stained sputum smear microscopy remained the most widely used diagnostic test in low-income countries and is the means by which universal access to diagnose TB and treatment initiation can be achieved [3].
Genotypic methods have advantages in terms of scaling up the programmatic management of TB delivering investigative results within a reasonable fast turnaround time, high throughput and fewer requirements for laboratory biosafety. Despite its advantages, the use of molecular tests for TB has been limited due to the complexities of DNA extraction, amplification and detection [4]. The development of the Xpert MTB/RIF assay platform was considered an important breakthrough in the fight against TB [4]. It was a molecular test which was simple and robust enough to be introduced and used outside conventional laboratory settings [4].
In Ethiopia, the need for simple, less expensive and robust diagnostic test in different population group including in People Living with Human Immuno Virus (PLHIV) is the concern of TB control program. People Living with Human Immuno Virus (PLHIV) are unable to produce enough sputum so that TB can be detected in their sputum. As a result Xpert MTB/RIF assay is recommended in such study setting.In Ethiopia including Addis Ababa, the accessibility of Xpert MTB/RIF assay for the diagnosis PTB was nearly 2% which limited its utilization in all health facilities [5]. On the contrary, in 59% of health facilities in Ethiopia, the only available diagnostic test was sputum smear microscopy and in 69%, at least some diagnostic tests were available including chest X-ray [5]. This study was aimed to compare the diagnostic performances of ZN-stained sputum smear microscopy and Xpert MTB/RIF assay in scaling up the utilization of Xpert MTB/RIF assay for the diagnosis of PTB in Addis Ababa, Ethiopia.
2. METHODS
2.1. Study Design and Setting
A facility based cross-sectional study design was conducted in Addis Ababa, Ethiopia from September 2016 to June 2017 to compare the diagnostic performances of ZN-stained sputum smear microscopy and Xpert MTB/RIF assay for the diagnosis of PTB against culture as a gold standard method. Based on 2007 census conducted by Ethiopian national statistics authorities, Addis Ababa has10 sub cities and 116 woredas (the lowest district of city administration) with an estimated total population of 3,384,569 and annual growth rate of 3.8% [6]. In the city, there are more 896 public and private health facilities, of which 101 public and 52 privates are delivering TB diagnostic services and Directly Observed Treatment Short Course (DOTS) [7]. Only 2% of health facilities in Ethiopia have Xpert MTB/RIF assay machine to diagnose TB and this holds true in Addis Ababa [5]. As a result sputum specimens are referred through postal system to the regional laboratory or lead hospitals where Xpert MTB/RIF assay machines are available and results sent back to the referred health facilities through a postal system of the existing national referral linkage map of the testing network.
2.2. Sample Size Determination
Convenient sampling technique was employed to determine the sample size based on the average national TB prevalence in general population of 2012 [8]. For convenience, the crude prevalence of TB was taken as 21% [8]. The following single population proportion formula was applied to obtain the actual sample size and the total sample size for the current study was 244 presumptive TB patients. However, two sputum samples were collected from each presumptive TB patient for Xpert and ZN-technique and the other for culture.
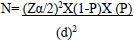
Where N = minimum sample size
Zα/2 = 1.96 at 95% Confidence Intervals (CI)
P = National TB prevalence
d= margin of error 0.05 at 95% CI
2.3. Study Subjects, Selection, Inclusion and Exclusion Criteria
Presumptive TB patients whose age are greater than or equal to eighteen years volunteered to provide sputum samples while undertaking TB diagnostic services in private and public health facilities in Addis Ababa during the study period. Follow up patients who were taking anti- TB treatment were not included in the study.
2.4. Test Procedures and Quality Assurances
Laboratory testing procedures and sputum specimen management were performed according to the stated Standard Operating Procedures (SOPs) of ZN sputum smear microscopy, Xpert MTB/RIF assay and L-J sputum culture [4, 9, 10]. Around 2-4 ml of sputum sample for Xpert MTB/RIF assay and smear microscopy, and 5-10 for L-J culture were collected in two separate falcon tubes and strict procedures were followed for reagents preparation, smears preparation and staining. The qualities of the prepared ZN-reagents were checked by staining with known positive and negative quality control sputum smear slides [9-11].
Sputum samples were decontaminated by N-Acetlyl-L-Cysteine-Sodium Hydroxide (NALC-NaOH) [9, 10]. The sterility of the prepared culture media was checked by incubating in an incubator for 48 hours at 37 ºC to see if there is no overgrowth of other contaminants [9, 10]. After quality check of the prepared culture media, 0.1 ml of decontaminated and distilled water re-suspended sputum samples were inoculated on L-J media [10]. According to its Standard Operational Procedures (SOPs), 2-4 ml sputum samples were processed for Xpert MTB /RIF assay [4].
2.5. Data Management and Statistical Analysis
The results of each test were entered into the excel sheet, checked for completeness, consistency and transferred to SPSS version 20 software for analyses. The sensitivity, specificity, PPV and NPV of ZN-technique and Xpert MTB/RIF were calculated against the MTB culture results as a gold standard.
3. RESULTS
3.1. Socio-Demographic Characteristics of Study Participants
From the total of 244 PTB presumptive patients enrolled in the study, 105 (43.03%) were female and 139 (56.97%) were male, with the mean age 36.23 and range of 68 year Table 1. Treatment histories of presumptive patients TB enrolled in the study were reviewed. Of the total presumptive patients enrolled in the study, 146 (59.84%) were new cases, 72 (29.51%) relapse, 20 (8.20%) treatment failure, 1 (0.41%) defaulter and 5 (2%) had no recorded previous treatment history.
| Age Group in Years | Male (%) | Female (%) | Total (%) |
|---|---|---|---|
| 18-27 | 38(27.34) | 38 (36.19) | 76(31.15) |
| 28-37 | 54 (38.85) | 33(31.43) | 87(35.66) |
| 38-47 | 21(15.11) | 19(18.10) | 40 (16.39) |
| 48-57 | 10(7.19) | 6 (5.71) | 16 (6.56) |
| >57 | 16(11.51) | 9(8.57) | 25(10.24) |
| Total | 139(100) | 105(100) | 244(100) |
| TB and HIV Co-Infections Among Patients Tested HIV | - | - | - |
| 18-27 | 7(31.82) | 6 (31.58) | 13 (31.71) |
| 28-37 | 5(23.81) | 2(28.57) | 7 (25) |
| 38-47 | 1(11.11) | 2(66.67) | 3 (25) |
| 48-57 | 1(33.33) | 0(0) | 1 (33.33) |
| >57 | 1(33.33) | 0(0) | 1(33.33) |
| Total | 15(25.86) | 10(34.48) | 25 (28.74) |
| Culture Positivity Rate Among Age and Sex | - | - | - |
| 18-27 | 25(65.79) | 20 (52.63) | 45 (59.21) |
| 28-37 | 34(62.94) | 9 (27.27) | 43 (49.43) |
| 38-47 | 12(57.14) | 5(26.32) | 17 (42.5) |
| 48-57 | 5(50) | 2(33.33) | 7(43.75) |
| >57 | 5(25) | 0(0) | 5(25) |
| Total | 81(69.23) | 36(30.77) | 117(100) |
From 244 PTB presumptive patients enrolled in the study, 166 (68.03%) were tested for HIV, of whom, males were 95 (57.23%) and female were 71 (42.77%). As illustrated in Table 1 below, HIV sero-positivity rate among the study participants tested for HIV was 54 (32.53%); 27 (28.42%) among male and 29 (35.53%) in female. From the total of 87 TB culture confirmed and HIV tested presumptive patients, 25 (28.74%) were co-infected with HIV; among them 15 (25.86%) were male and 10 (34.48%) were female.
From the total of 244 PTB presumptive sputum samples cultured on L-J media, 117 were found culture positive. As illustrated in Table 1 below, culture positivity rate was highest among age groups of 18 to 37 years.
3.2. Performances of ZN Stained Direct Sputum Smear Microscopy, Xpert MTB/RIF Assay Versus Culture Results Gold Standard Test
From 244 sputum samples analyzed by culture and ZN-stained direct sputum smear microscopy, 80 (32.79%) were positive by both ZN- stained direct sputum smear microscopy and culture methods; 6 (2.46%) were smear-positive but culture negative;121 (49.2%) were negative by both methods and 37 (15.16%) were culture positive but smear negative. On the contrary, from a total of 244 sputum samples analyzed by Xpert and L-J culture, 104 (42.62%) were positive by both methods, 23 (9.43%) were positive by Xpert but culture negative, 104 (42.42%) were negative by both Xpert and MTB culture while 13 (5.33%) were negative by Xpert MTB/RIF assay but culture positive illustrated in Table 2.
| Diagnostic Tests Under Evaluation | Mycobacterium Culture Results | - | ||
|---|---|---|---|---|
| - | Positive (%) | Negative (%) | Total (%) | |
| ZN-Results | Positive (%) | 80(32.79) | 6(2.46) | 86(35.25) |
| Negative (%) | 37(15.16) | 121(49.59) | 158(64.75) | |
| Total | 117(47.95) | 127(52.05) | 244(100) | |
| Xpert MTB/RIF Results | Positive (%) | 104 (42.62) | 23(9.43) | 127(52.05) |
| Negative (%) | 13 (5.33) | 104(42.42) | 117(47.95) | |
| Total | 117(47.95) | 127(52.05) | 244 (100) | |
3.3. Sensitivity, Specificity, Positive and Negative Predictive Value of ZN- Technique and Xpert MTB/RIF Assay
In this study, the sensitivity, specificity, PPV and NPV of ZN-technique and Xpert MTB/RIF were calculated against the gold standard culture. The sensitivity, specificity, PPV and NPV by ZN-sputum smear microscopy were 68.38% (95% CI: 59.13 to 76.66), 95.28% (95% CI: 90.00% to 98.25%), 93.02% (95% CI: 85.81% to 96.71%) and 76.58% (95% CI, 71.42% to 81.06%) respectively. The diagnostic yield and accuracy of the test method were 32.79 and 35.25, respectively. The measure of positive agreement between the ZN and the gold standard results was substantial with a kappa coefficient (k= 0.650). The sensitivity, specificity, PPV and NPV of Xpert MTB/RIF assay were 88.89% (95% CI: 81.75% to 93.95%), 81.89% (95% CI: 74.08% to 88.16%), 81.89% (95% CI: 75.65% to 86.81%) and 88.89% (95% CI: 82.64% to 93.08%) respectively. The diagnostic yield and accuracy of the test MTB/RIF assay were 42.62% and 52.05% respectively. The measure of agreement between Xpert MTB/RIF assay and culture results was substantial with kappa coefficient (k= 0.743).
4. DISCUSSION
The present study evaluated the diagnostic performances of ZN-stained sputum smear microscopy and Xpert MTB/RIF assay test for the diagnosis of PTB by using MTB culture as the gold standard. The sensitivity, specificity, PPV value and NPV of Xpert MTB/RIF assay were 88.89%, 81.89%, 81.89% 88.89% and of ZN-stained sputum smear microscopy, these were 68.38%, 95.28%, 93.02%, 76.58% respectively.
The sensitivity of Xpert MTB/RIF assay in the present study was almost similar to study conducted in India, Nepal, Pakistan and Italy with sensitivity of 86.8%, 86.5%, 90.1% and 85.4%, respectively [12-15]. However, it was higher than 83.9% reported from Thailand [16]. The specificity of Xpert MTB/RIF assay in the present study was much lower compared to study in Pakistan showing specificity of 98.3% [13] and 90% specificity from India [12]. This study includes both smear positive and negative sputum while the study of Thailand was on smears negative PTB [19].
The sensitivity of ZN-stained sputum smear in the present study was higher than 61.1% reported from South Africa, Cape Town [17]. This might result from the sample size (221) in the study of Cape Town and study population. The present study was conducted on 244 sputum samples that were PTB and MRD-TB presumptive as well as all treatment categories (new, relapse, retreatment cases) as a source of sputum. However, the sensitivity of the present study was comparable with the study conducted in Pakistan showing sensitivity of 67.5% [13].
The specificity of ZN-stained direct sputum smear microscopy (95.28%) was relatively higher compared to the study conducted in Pakistan showing specificity (91.4%) [13, 18].The difference might be attributed to sample size and type. In the present study, 244 samples were analyzed, of whom all were sputum while in the study of Pakistan, 387 sputum and 7 bronchial wash were analyzed [13, 18, 20].
CONCLUSION
With the evidences from the result, this study concludes that the sensitivity of Xpert MTB/RIF assay was better than ZN-stained direct sputum smear microscopy for the diagnosis of pulmonary tuberculosis.
LIST OF ABBREVIATIONS
| CI | = Confidence Interval |
| DOTS | = Directly Observed Treatment- Short course |
| PLHIV | = People Living with Human Immunodeficiency Virus |
| L-J | = Lowenstein Jensen media |
| PTB | = Pulmonary Tuberculosis |
| MTB | = Mycobacterium Tuberculosis |
| PPV | = Positive Predictive Value |
| NALC-NaOH | = N-Acetlyl L-Cysteine-Sodium Hydroxide |
| NPV | = Negative Predictive Value |
| RIF | = Rifampcin |
| SOPs | = Standard Operational Procedures |
| SPSS | = Statistical Package for Social Science |
| TB | = Tuberculosis |
| ZN | = Ziehl-Neelsen |
AVAILABILITY OF DATA AND MATERIALS
All data were presented in the result parts of the manuscript.
FUNDING
This study was not supported from any funding organization
AUTHOR(s) CONTRIBUTION
BDT led sputum samples collection process, analysis and writing up of the manuscript. DMD reviewed and evaluated manuscript. All other authors were participated in organizing, analysis, interpretation of results and approved the final version of this manuscript.
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
Before conducting this research, permission was obtained from Addis Ababa City Administration Health Bureau Public Health Research and Emergency Management Core Processes ethical review committee with a reference # 6023/227.
HUMAN AND ANIMAL RIGHTS
Not applicable.
CONSENT FOR PUBLICATION
Before the research work, verbal consent was obtained from each patient.
CONFLICT OF INTEREST
The author declares no conflict of interest, financial or otherwise.
ACKNOWLEDGMENTS
The authors would like to thank Addis Ababa City Administration Health Bureau and health facilities in the city for their cooperation. We would like to thank medical laboratory professionals in these health facilities for collecting the sputum samples, post-men who brought the samples to Addis Ababa regional laboratory for analysis.


